Moles / Skin cancer screening
 have them checked regularly and prevent skin cancer
have them checked regularly and prevent skin cancer
They can occur on any part of the body, take on different shapes and colours and are different in size: the small, mostly brown, spots and elevations on the skin are colloquially referred to as moles or liver spots.
As a rule they are completely harmless but may affect the patient’s aesthetic appearance. This article will provide you in a nutshell with information on why moles should be checked periodically, how dangerous they actually are, and what removal options you can consider.
This post will cover:
-
How is artificial intelligence used in skin cancer screening?
-
Are mole checks using dermoscopy and full-body scanners the same everywhere?
What are moles and how do they develop?
Moles can appear at birth or later in life. Hereditary factors, the extent and intensity of solar radiation and skin type are causally involved in their development. Moles are a collection of pigment-forming nevus cells that rise from the deeper layers of the skin and multiply in the upper layers. As a rule, they are not dangerous, yet they can lead to alternations or degeneration of the skin and melanoma can develop that can triggers other skin cancers.
Periodic examinations, which we carry out in our practice in Vienna, are critical for early diagnosis.
What causes moles?
Their appearance is not due to a single factor. If they are commonly present in the direct family (parents, grandparents), then probability of occurrence increases.
Skin type plays a major role. Generally speaking, the lighter the skin, the higher the number of moles. In people with dark skin, they usually occur in a smaller number.
Melanin is an important factor in the development of moles and contributes significantly to the dark colouring of the skin.
How dangerous are moles?
One associates moles with skin cancer. Currently, the number of people suffering from skin cancer is increasing in Austria. Recognised early, skin cancer is easily curable. As the disease can also affect younger patients, periodic mole control or skin cancer screening is also recommended for this age group. There are certain danger signs that should be observed. For the first self-examination, you can follow the ABCDE rule:
- Asymmetric changes
- Boundaries that are irregular
- Colour, not uniform pigmentation
- Diameter more than 5 mm
- Elevation
The above is used as an initial tool to identify suspicious moles. A medical consultation is required if at least two of the five points apply.
How is skin cancer screening done?
 Skin cancer prevention is extremely important to us, which is why we have brought high technology to Vienna. In our medical center, we document your entire skin surface with a full-body scanner. Your skin is recorded in high quality using full-body cartography and video dermatoscopy. The image material of your entire skin surface is then analyzed with artificial intelligence in order to compare your moles with 135,000 comparative data sets to assess the risk probability for skin cancer. The image material is saved so that your skin can be compared over time and conspicuous developments can be identified.
Skin cancer prevention is extremely important to us, which is why we have brought high technology to Vienna. In our medical center, we document your entire skin surface with a full-body scanner. Your skin is recorded in high quality using full-body cartography and video dermatoscopy. The image material of your entire skin surface is then analyzed with artificial intelligence in order to compare your moles with 135,000 comparative data sets to assess the risk probability for skin cancer. The image material is saved so that your skin can be compared over time and conspicuous developments can be identified.
In a second step, particularly conspicuous moles are additionally documented with a special camera in 140x magnification. Even the smallest changes in a mole can be identified with this instrument. In this way, a painless and non-invasive distinction can be made quickly between harmless and suspicious changes.
This gives you multiple benefits: Artificial intelligence and medical expertise combined. In addition, no doctor could ever remember all the moles on your body and detect changes between examinations. Thanks to the technological support, the medical ability to recognize conspicuous moles is significantly improved.
Based on your individual mole status, we recommend a control schedule that is tailored to you. This can be a period of 2 years until the next appointment, but in some cases - especially with cancer follow-up care - it may be necessary every 3 months. Only with the help of the computer-aided follow-up images created during these check-ups can moles that change be diagnosed early and reliably.
We are proud that we are the first and only practice in Vienna to offer this technology. Since skin cancer prevention is so important to us, this new technology is offered at the same price as the previous system, which exclusively used a hand scanner.
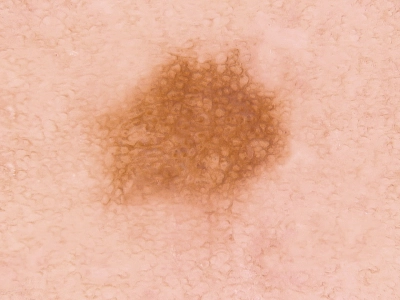
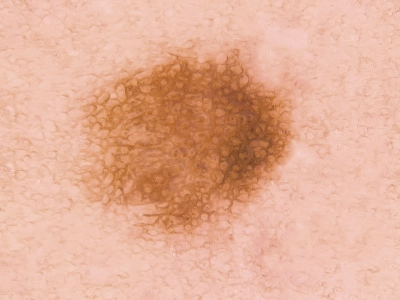
When do you have to have a mole treated?
As long as a birthmark is not conspicuous, treatment is not required. If it is not clear in the course of an examination whether it is benign or malignant then it should be removed and examined histologically to be sure. Most moles are however removed for aesthetic reasons, especially if they are on the face or other visible areas.
Which types of moles are there?
Moles occur in different forms. It is good to know these in order to respond to changes in a timely manner. The classic forms are:
- Congenital moles (congenital nevus): they are, as the name says, already present at birth. They come in different shapes, sizes, and colours, and usually become visible in the first year of life. For them, the risk is slightly higher than for the moles which appears later in life. Hairy moles should be watched closely. Statistically there is an increased risk when the mole is larger than one centimetre in diameter.
- Common birthmark (nevus) are single coloured and regularly limited. Almost all people have these moles. In Northern Europe an average person has about 30 to 40.
- Elevated mole (papillomatous nevus): This type of mole looks rather scary, sometimes hair grows out of it. It is single-colored and represents a rather cosmetic problem because of the rough, somewhat raised surface and the hair.
- Unusual birthmark (atypical or dysplastic nevus): The appearance is close to the malignant melanoma. It has a diameter of more than 5 mm, has different colours with a frayed edge, flat or raised. When such moles occur, a dermatologist should be consulted urgently as the risk of getting melanoma is higher.
- Blue birthmark (blue nevus): The birthmark is gray-blue in colour, flat or elevated. The colour is created by refraction. The actual birthmark is located in deeper skin layers. This type of birthmark can change and should be kept under observation.
Do not take any risks
If you notice unusual moles; especially those that grow fast, an examination is strongly recommended. You are welcome to make an appointment at our practice. Book an appointment.
How are moles removed?
Whether the removal of a mole is recommended and how it should be done, will be discussed with you after a thorough examination. All removed moles are examined histologically by a Pathologist (this may take several weeks) to exclude any risk. The surgical removal itself is done under local anaesthesia and is painless. What is important to us is the cosmetically demanding removal of all skin lesions and the avoidance of unsightly scarring. In certain moles (for example, papillomatomatous nevi or fibroids), removal can be gentle with the high-efficiency Erbium laser or cautery (electricity).
How are moles and skin cancers related?
Cancers of the skin are grouped under the name "skin cancer". Two types can be distinguished:
• White skin cancer (basal cell carcinoma, squamous cell carcinoma, actinic keratosis): they form virtually no metastases.
• Black skin cancer (malignant melanoma): metastasises already in the early phase and changes can hardly be detected by visual observation alone.
It should be pointed out again that intensive sun exposure and insufficient sun protection contribute to the development of moles and white and black skin cancer.
How can actinic keratosis or chronic photodamage be treated?
Actinic keratoses are white skin cancer precursors and develop after chronic light damage. Treatment is important because the precursors can develop over a period of months or years to skin cancer. In our practice, we can remove these precursors with the latest high-efficiency precision laser, the Erbium laser. Other options to treat these precursors include liquid nitrogen or curettage. Another option is the daylight PDT in which a medical cream, combined with sunshine, triggers a chemical reaction which leads to the rejection of altered cells. With this therapy larger areas can be treated effectively and painlessly.
Regular mole / skin cancer screening is especially important. The earlier a disease is detected, the better the chances of recovery.
Are mole checks using dermoscopy and full-body scanners the same everywhere?
No. Modern mole screening today relies on a wide range of technical systems. Early full-body scanners were an important step forward because they allowed the entire skin surface to be documented for the first time. However, newer generations of scanners and dermatoscopes offer significantly more: they combine high-resolution imaging with AI-supported analysis, making it easier to detect even subtle changes at an early stage.
For us, it is essential to work with the most up-to-date and precise technologies. This is why we use systems that both map the entire skin and analyse individual moles in detail — ensuring the highest possible diagnostic accuracy.
I have been diagnosed with melanoma – what now?
The next steps depend on the stage of your tumor, particularly the tumor thickness. Immediately after the diagnosis, your treating physician will inform you whether further excision, imaging, blood tests, or a lymph node biopsy are necessary. Based on this, a personalized follow-up plan will be created for you.
For patients at higher risk, a full-body screening using the FotoFinder ATBM (a total body mapping system) is strongly recommended. This advanced technology is available at our clinic at Vienna Central Station.
In addition to the required skin cancer screenings, we also offer blood tests (tumor markers) and lymph node ultrasounds directly at our practice. Dr. Schreiber and Dr. Hauser have years of experience from leading cancer centers in Germany and are fully up to date with the latest medical standards.
We can often perform follow-up excisions (re-excisions) directly in our in-house procedure rooms without long waiting times. If you have recently received a diagnosis, please don’t hesitate to contact us. We are here to support you and guide you through the next steps.
Our range of services for skin cancer screening and mole control includes:
- Information and advice on skin type and personal sunscreen needs.
- Clinical examination with state-of-the-art instruments: dermatoscope, digital dermatoscope, Foto-Finder® including the Bodyscanner (documentation in chronological order)
- Removal of moles and other benign or malignant lesions by gentle laser or cosmetic surgery.
- Surface treatment of skin cancer precursors using Daylight PDT and laser.
Dr. Christina Hauser and Dr. Antonia Schreiber have both worked in tumor centers and are trained in performing lymph node ultrasound. Lymph node ultrasound is recommended in follow-up guidelines for patients with melanomas of greater depth.
FAQ – Moles & Skin Cancer Screening
Here you will find answers to the most important questions about moles, skin cancer risk factors, and the latest methods for early detection of suspicious changes.
-
What are moles and how do they form?
Moles are clusters of pigment-producing cells that can be present at birth or develop over time.
-
Why should I have my moles checked regularly?
Regular check-ups help detect dangerous changes early and prevent and treat skin cancer.
-
How is a mole check performed?
We take a look at your whole skin and also use full-body scanning, video dermatoscopy and AI-assisted analysis.
-
What types of moles exist?
There are many different types of moles. The most common include:
– Congenital moles (congenital nevi) – present at birth or shortly after.
– Acquired moles – develop during life due to genetics and UV exposure.
– Elevated moles – dome-shaped, mostly benign, and usually slow-growing.
– Atypical or dysplastic moles – irregular in shape and colour, with a higher risk of change into a melanoma.
– Blue nevi – blue-grey pigmented moles, often slightly raised.
There are also many additional subtypes that should be assessed by a dermatologist. -
Which ABCDE warning signs are important?
Asymmetry, irregular border, multiple colours, diameter > 5 mm, evolving or elevated changes.
-
When should a mole be removed?
If it changes, appears suspicious or is cosmetically bothersome.
-
How are moles removed?
Surgically under local anesthesia, or for benign lesions, by laser or cauterization.
-
How are moles related to skin cancer?
Some melanomas arise from moles; UV exposure increases the risk.
-
What happens if a melanoma is diagnosed?
Treatment depends on tumour thickness and stage of disease; ongoing follow-up is essential.
-
How can I prevent dangerous moles?
Use sun protection, avoid sunburns, and get annual dermatologist check-ups.
You are welcome to make an appointment for a first consultation in our practice in Vienna.Book an appointment.



